Frequency Variation and Dose Modification of Benznidazole Administration for the Treatment of Trypanosoma cruzi Infection in Mice, Dogs, and Nonhuman Primates
Chet Joyner receives $1.1 million grant to study malaria vaccine
RESEARCH WILL BE IN COLLABORATION WITH YALE UNIVERSITY Chet Joyner, PhD, a faculty member in the Center for Vaccines and Immunology and the Center for Tropical and Emerging Diseases in the College of Veterinary Medicine (CVM) at the University of Georgia, is the recipient of a $1.1 million grant from Open Philanthropy to perform preclinical …
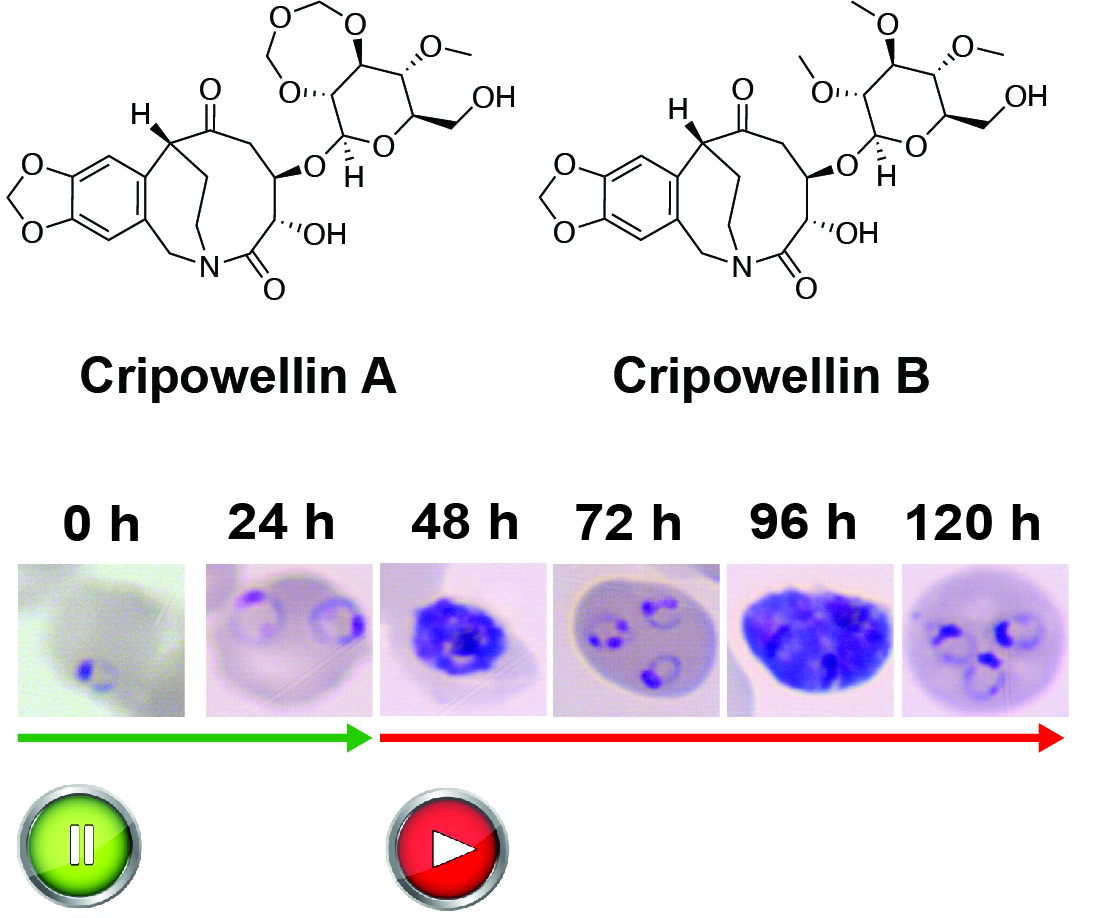
Cripowellins Pause Plasmodium falciparum Intraerythrocytic Development at the Ring Stage
Cripowellins from Crinum erubescens are known pesticidal and have potent antiplasmodial activity. To gain mechanistic insights to this class of natural products, studies to determine the timing of action of cripowellins within the asexual intraerythrocytic cycle of Plasmodium falciparum were performed and led to the observation that this class of natural products induced reversible cytostasis in the ring …