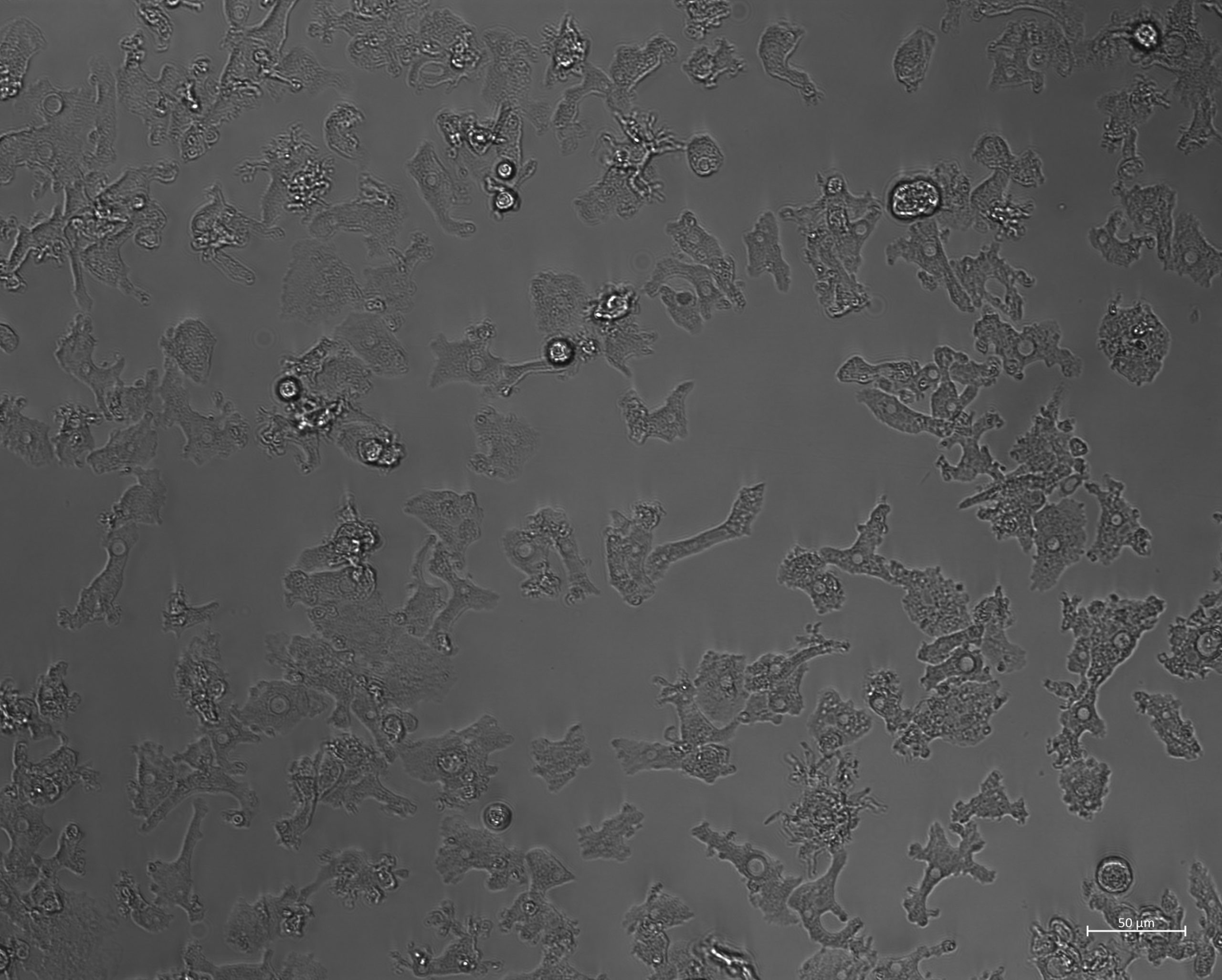
Differential Growth Rates and In Vitro Drug Susceptibility to Currently Used Drugs for Multiple Isolates of Naegleria fowleri
The free-living amoeba Naegleria fowleri, which typically dwells within warm, freshwater environments, can opportunistically cause primary amoebic meningoencephalitis (PAM), a disease with a mortality rate of >97%. The lack of positive treatment outcomes for PAM has prompted the discovery and development of more effective therapeutics, yet most studies utilize only one or two clinical isolates. …